Posted on April 13, 2016 by SMPC - Painful Conditions
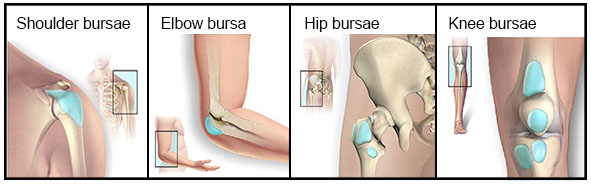
Certain areas of the musculoskeletal system experience significant stress from everyday living. Fluid filled sacs, called bursae (bursa) cushion the bones, tendons and muscles near your joints. Unfortunately bursae can become inflamed and irritated and this is call bursitis. Bursitis often occurs near joints that perform frequent repetitive motion. The most common sites for this to occur are the hips knees, shoulders and elbows.
Diagnosis
The patient with bursitis will complain of well-localized pain in the shoulder, hips or other joints. The pain may travel from one of these areas into the arm or thigh. When the doctor examines the patient, he or she will look for swelling and tenderness over the locations of the bursa. Doctor can often diagnose bursitis based on the medical history and physical exam. If further testing is needed, the doctor my order x-rays. X ray images can’t positively establish the diagnosis of bursitis but they can help to exclude other cause of your discomfort. The bulk of bursa inflammation occurs in the soft tissue, which cannot be seen on X-ray.
Treatment
There are many treatment for bursitis. In the early stages, an anti-inflammatory drug will frequently help the problem. Ice should can also be applied over the inflamed area several times during the day to assist with swelling. It is important to rest the affected area. For example, avoid elbow pressure by not leaning on the elbow or if the right hip is affected, try to sleep on the left side. If these treatment strategies fail to work, the doctor may inject an anti-inflammatory drug and /or corticosteroid directly and into the bursa. These drugs are very useful for the relief of inflammation. These drugs generally bring rapid pain relief and in many cases, one injection is all you need. Although if more than one injection is needed, these medications can only be used a few times each year. Physical therapy may be ordered to strengthen the muscles in the affected area to ease pain and prevent recurrence. The physical therapist may use ultrasound and soft tissue manipulation that can sometimes be helpful. Sometimes an inflamed bursa must be surgically drained.
Download the information sheet in pdf
Posted on April 13, 2016 by SMPC - Painful Conditions
Peripheral neuropathy is a burning or aching pain due to nerve diseases. The pain can either be constant or intermittent and most often occurs in the arms or legs; however, it has been known to occur in the trunk, abdomen, head and neck. The pain can occur from irritation of one nerve or from several nerves. Generally, peripheral neuropathies are a consequence of diabetes, alcoholism or other neurological diseases.
Diagnosis
Doctors will use a physical examination to confirm the area involved. Neurological examinations can sometimes reveal loss of sensation to pinprick or to hot and cold temperatures. Weakness is sometimes noted in the affected extremity. Reflexes may be affected and there may be changes in the skin over the region. Evaluations of peripheral neuropathies usually involve tests appropriate for the primary disease, which doctors suspect is causing the problem such as diabetes. Evidence of nerve damage can sometimes be demonstrated with electrical nerve testing. Doctors who treat the pain as peripheral neuropathy will often use a nerve block procedure to help diagnose the problem.
Treatment
For some patients with peripheral neuropathy, the use of oral non-steroidal anti- inflammatory medications along with traditional pain medications can be helpful. For others, special medications help directly with nerve pain. These medications are often started at low doses and gradually increased until the desired affects are reached. Long-term relief can often be obtained with the use of therapeutic nerve blocks. These include injections of anesthetic medications along with anti-inflammatory medication around the painful nerves. The injections are usually performed in a short series over several weeks until symptoms subside or a plateau is reached in the treatment. If helpful, these injections can be repeated at appropriate intervals.
Nerve stimulation techniques can be helpful in certain types of peripheral neuropathy. Stimulation can either occur on the skin over the affected region, or in some cases, with stimulator electrodes placed surgically around the nerves or in the spine at the origin of the affected nerves. Although physical therapy is not usually helpful in relieving the pain from peripheral neuropathy, therapeutic exercises can help restore loss of function and allow patients to lead more active lives. In addition, behavioral modification techniques or biofeedback training with muscle relaxation exercises can help patients be less sensitive to the irritation from the affected nerves.
Download the information sheet in pdf
Posted on April 13, 2016 by SMPC - Painful Conditions
This disorder is a type of headache with discomfort noted at the back of the head, beginning at the base of the skull and radiating upward toward the top of the head. The symptoms can occur on either side of the head, or it can include both sides. The symptoms can be sharp, spasm-like pains that occur at different intervals. It is caused from irritation of the occipital nerves, which begin at the back of the head and extend to the top of the head. Occipital neuralgia is caused by inflammation or injury to these nerves. It can also be caused by excessive muscle tension in the muscles at the back of the head through which these nerves pass.
Diagnosis
A physical examination will usually show signs of increased tenderness in the tissues at the base of the skull and at the top of the spine. Doctors can use X-rays to determine whether there is any narrowing of the vertebra at the top of the spine, where the occipital nerves pass to the back of the head. The best test to confirm occipital neuralgia is an injection of anesthetic, called a nerve block, given at the base of the skull around the occipital nerve itself. If blocking the occipital nerve results in resolution of the symptoms, the diagnosis of occipital neuralgia is usually confirmed.
Treatment
One of the greatest concerns to doctors treating this problem is to make sure that these symptoms do not indicate an increase in intracranial pressure within the skull, which could signal a vascular, infectious or other significant problem. Some patients will find temporary relief from the pain with the use of non-steroidal anti-inflammatory drugs and muscle relaxants. Physical therapy exercises will also provide some limited effectiveness. Doctors believe the best approach for long-term relief is the use of nerve block treatments. In some cases, an injection of local anesthetic combined with medication to reduce inflammation can result in long-term relief following a series of treatments. At times, the pain at the base of the skull is related to other disorders or arthritis in the joints of the upper portion of the spine. Doctors may use nerve block injections around these structures to help in the treatment of occipital neuralgia. Surgery can sometimes provide relief for several months, but most patients find the pain may return. Surgery is usually reserved as a last option. Some patients will find additional help through a combination of muscle relaxation techniques, known as biofeedback, in conjunction with physical therapy that focuses on manual therapy to the muscles at the back of the neck and head. Newer block treatments at the occipital nerves can also be utilized for long-term treatment at appropriate intervals.
Download the information sheet in pdf
Posted on April 13, 2016 by SMPC - Painful Conditions
While surgery and surgical procedures have become specialized and involve as little tissue damage as possible, they nonetheless involve the cutting, removing and suturing of skin, muscles, nerves and other structures. Therefore some surgical procedures can cause chronic pain due to the trauma of the procedure. Post thoracotomy pain is an example of pain associated with the surgical procedure. Doctors define post thoracotomy pain as pain that returns or persists around the surgical incision for at least two months after the surgery. The pain is generally located along the chest wall. Patients who have post thoracotomy pain describe it as achy-like, burning or sharp. Pain can result from entrapped nerve fibers in the area of the scar tissue.
Sometimes a neuroma or painful lump of nerve tissue can form at the tip of a nerve in the chest wall where it has been cut during surgery. Pain from the muscles in the chest or shoulder may contribute to post thoracotomy pain syndrome as well. If the thoracotomy was performed to remove a tumor involving the lining of the chest or the chest wall, continued pain may indicate tumor recurrence.
Diagnosis
Doctors will use a physical examination to confirm a painful area near the surgical scar and to map the area of irritation. A CT scan of the chest sometimes helps determine if a tumor has reoccurred. Doctors may use a kind of nerve block or injection of anesthetic medications around a neuroma or nerve in the chest wall to help confirm the diagnosis.
Treatment
Some patients benefit from oral non-steroidal anti-inflammatory medications with the addition of pain medicine. Long-term relief is often obtained from the use of nerve blocks given into a neuroma, local anesthetics and anti-inflammatory medications. Other nerve block treatments can be given along the path of the various nerves in the chest, which contribute to the pain after thoracotomy surgery. Sometimes nerve stimulation procedures are used to help relieve pain along the chest wall. Physical therapy exercises may be utilized to regain the ability to perform normal daily activities.
Download the information sheet in pdf
Posted on April 13, 2016 by SMPC - Painful Conditions
Shingles is an infection of an individual nerve root by the same virus that causes chicken pox, also known as the herpes zoster virus. The disease can be painful and can develop almost anywhere in the body, but is most commonly displayed on the face, chest and abdomen.
A day or two after the pain begins; a characteristic rash erupts, which is composed of small fluid-filled blisters on top of reddened skin. The blisters are limited to a band on the right or left side of the body. If the rash crosses over the middle of the body it is not shingles because the virus affects one nerve corresponding to an area of the skin. Each cutaneous or skin nerve in the human body stays on the right or left side and does not cross over. Initial infection of the shingles virus occurs when chicken pox is contracted as children or young adults. The body’s immune system forces the virus to settle in an inactive form inside the nerve cells. When the chicken pox virus reactivates, it moves down the nerve fibers to the skin and the rash erupts. In addition to the skin, the nervous system is involved. In fact, if the virus attacks the optic nerve of the eye, it may leave the patient with temporary blindness.
In most patients, after the eruption of shingles, the rash will heal and the pain will subside after a period of three to five weeks. However, there are exceptions. In older patients there is a greater risk the virus can actually leave permanent nerve damage, causing pain long after the rash is healed. In some patients, the pain may persist for the rest of their lives.
Treatment
Medical science is now developing antiviral drugs. These are similar to antibiotics that were developed in the 1950’s to treat bacterial infections. One of the first antiviral drugs developed was acyclovir. This drug can help resolve herpes infections. As soon as the rash breaks out, acyclovir is prescribed in large doses for a period of approximately 10 days. This can help alleviate the attack and prevent permanent nerve damage in some patients.
Additionally, early intervention with nerve blocks done by pain physicians can also prevent the development of post-herpetic neuralgia. Post-herpetic neuralgia is the name given to the painful condition that exists long after the viral infection is over. Combination therapy of the acyclovir and nerve blocks is the most effective treatment strategy for preventing this painful development.
There is treatment for patients suffering from post-herpetic neuralgia. Drugs used to treat seizures, such as Tegretol and Dilantin, can be of some help. Antidepressants are used to treat post-herpetic neuralgia as well. The antidepressants raise levels of chemicals in our brain that are the body’s natural mood elevators. These mood elevators also raise levels of endorphins in the brain, which are the body’s natural narcotics. Consequently, by taking antidepressants, we can elevate the body’s internal narcotics without having to rely on narcotics prescribed by the doctor. Therefore, antidepressants are superior to narcotics because dependence can develop in narcotics.
Download the information sheet in pdf

